Platelet-rich plasma, or PRP, has received significant attention in sports medicine and pain management over the last decade. You may have read about it in connection with professional athletes, joint pain, or tendon problems. If you are in Woodland Hills and weighing whether PRP could help with your pain, this guide walks through what PRP actually is, what the evidence currently supports, and how a pain management practice approaches the question of whether you are a good candidate.
What Is PRP?
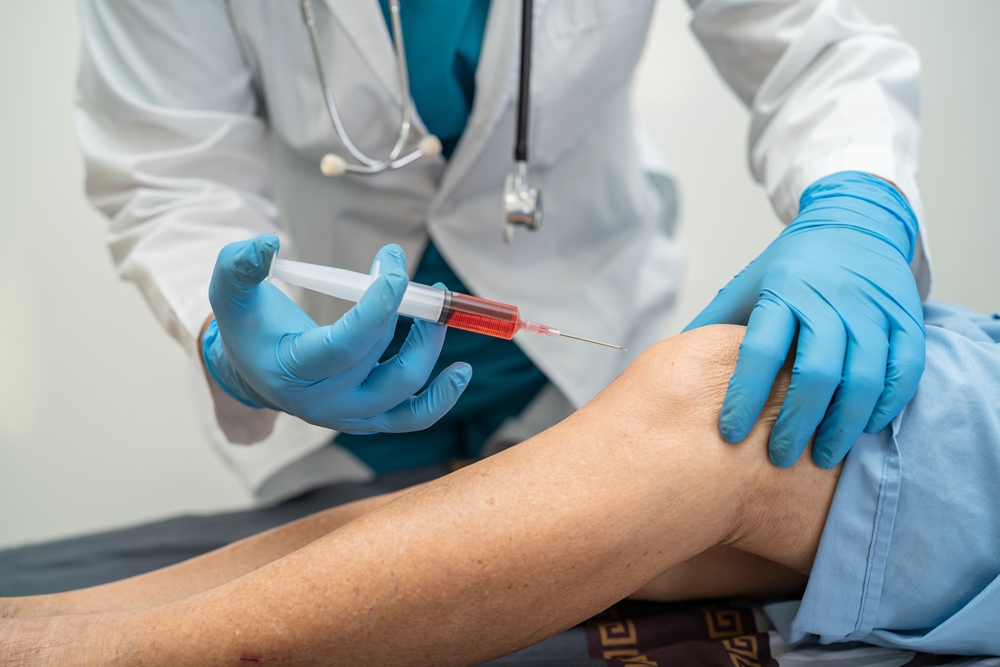
Platelet-rich plasma is a concentrated preparation of your own blood. A small sample of blood is drawn, processed in a centrifuge that separates out the platelet-rich portion, and then injected into the area being treated. The premise is that platelets contain growth factors that may contribute to tissue healing when concentrated at the site of a chronic injury.
Because PRP is made from your own blood, there is no concern about rejection or cross-reactivity in the way there would be with a donor product. The safety profile is generally favorable.
What PRP Is Used For
PRP is most commonly used in pain management and orthopedics for:
- Knee osteoarthritis
- Chronic tendon problems (tennis elbow, golfer’s elbow, patellar tendinopathy, rotator cuff tendinopathy)
- Certain ligament injuries
- Some joint pain conditions that have not responded to other treatments
The field’s understanding of which conditions respond best to PRP continues to evolve. Evidence is stronger for some uses than others, and outcomes can vary considerably between patients even for conditions where PRP is well-established.
What PRP Is Not
A few points worth being clear about:
PRP is not the same as stem cell therapy. These are different treatments with different mechanisms. Some clinics market them together; they are separate things.
PRP is not a cure for osteoarthritis. It may provide pain relief and functional improvement for some patients with knee or other joint arthritis, but it does not reverse cartilage loss or rebuild the joint.
PRP is not always covered by insurance. Many health plans consider PRP investigational for most uses and do not cover it. Patients typically pay out of pocket. Ask about costs upfront.
PRP is not the right treatment for every pain problem. Many conditions respond better to other interventional procedures, and an evaluation should come before any decision to pursue PRP.
Who Is a Good Candidate?
A pain management physician generally considers PRP for patients who:
- Have a condition that has some evidence supporting PRP use
- Have tried appropriate conservative treatments without adequate improvement
- Are not yet candidates for, or want to defer, more invasive options like surgery
- Understand that results vary and that PRP is not a guaranteed solution
- Are in reasonably good general health
- Are not on blood thinners that would preclude the procedure (or can safely stop them, with their prescriber’s input)
Patients who are unlikely to be good candidates include those whose pain has a clear structural cause that PRP cannot address, those in the midst of an infection, those with certain blood disorders, or those whose condition falls outside the range where PRP has reasonable supporting evidence.
What the Procedure Involves
A typical PRP session involves:
- A small blood draw, usually from an arm vein
- Processing of that sample in a centrifuge to isolate the platelet-rich portion (this takes several minutes)
- Cleansing the area to be treated and applying a local anesthetic
- Injection of the PRP, often with image guidance for precise placement
- A short post-procedure observation period before you leave
The procedure is outpatient. Some patients experience a day or two of soreness at the injection site. Specific activity guidance depends on the area treated and your individual situation.
Results are not immediate — PRP works on a different timeline than a steroid injection. Benefit typically develops over weeks.
How PRP Fits Into a Broader Pain Management Plan
PRP is rarely a standalone treatment. For most conditions where it is used, it is one component of a plan that also includes physical therapy, activity modification, and sometimes other treatments. The reasoning is straightforward: if PRP reduces pain, physical therapy tends to be more productive during that window, and sustained improvement usually depends on both.
Our Approach at Southwest Pain Management
At our Woodland Hills clinic, we approach PRP as one tool among several. Before recommending PRP, we perform a careful evaluation to confirm the diagnosis, review what you have already tried, and discuss whether PRP has a reasonable chance of helping your specific situation. We are honest about the evidence and about realistic expectations.
We do not recommend PRP when another treatment is more likely to help. And we discuss costs and insurance coverage upfront — most patients pay out of pocket, and the cost should be part of the decision.
Frequently Asked Questions
Is PRP covered by insurance? Most insurance plans consider PRP investigational for most uses and do not cover it. Patients typically pay out of pocket. Verify with your specific insurance plan before the procedure.
How long until I feel relief after PRP? Unlike a steroid injection, which often works quickly, PRP typically works on a slower timeline. Benefit, when it occurs, often develops over several weeks.
How many PRP treatments will I need? This varies. Some patients benefit from a single treatment; others require a series. Your physician will discuss what is reasonable for your situation before you start.
Is PRP the same as stem cell therapy? No. PRP uses a concentrated portion of your own blood. Stem cell therapy uses a different type of cellular product. They are separate treatments with different mechanisms and different regulatory considerations.
What are the risks of PRP? Because PRP uses your own blood, it has a favorable safety profile. Like any injection, it carries a small risk of infection, bleeding, or injection site discomfort. Your physician will review the specific risks relevant to your procedure.
Who should not get PRP? PRP may not be appropriate for patients on certain blood thinners, those with active infections, patients with certain blood disorders, and those whose condition is unlikely to respond to PRP.
Talk to a Specialist About Whether PRP Is Right for You
Contact Southwest Pain Management to request a consultation at our Woodland Hills clinic and discuss whether PRP or another treatment is the best next step.
Our Mission
The mission of Southwest Pain Management is to empower you to restore function, decrease pain, and live your life to its fullest.
Contact Us

